|
|
Atrial Fibrillation
Go here for an "X-Plain it" Interactive Health Tutorial on
Atrial Fibrillation
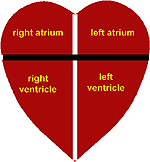
The heart is a
pump which is divided into two sections, the atria and
ventricles, and into two halves the left and right. This means
that the heart is divided into 4 chambers. The atria pump
blood into the ventricles and thus have a relatively small job
to do, and the ventricles pump blood around the body and thus
take on most of the work. The atria are therefore thinner and
smaller than the muscular ventricles. The right heart pumps
blood through the lungs to get oxygen into it and the left
heart pumps blood around the body including the
brain. Normally the atria pump
blood into the ventricles before the ventricles then pump
blood around the body. They therefore work in sequence. This
sequence is controlled by an electrical system. A small bunch
of cells situated at the top of the heart, the sinus node (SN)
sends an electrical impulse out at about 60 to 70 times a
minute (hence your heart rate is 60 to 70). This gets faster
if you need your blood to move through your body more quickly,
for example if you are exercising. This electrical impulse
then washes like a wave across the atria from right to left
being conducted from cell to cell and making the cells
contract causing the atria to squeeze (video animation might
be good here if we can get it commissioned). The atria and the
ventricles are insulated from one another (black line) so when
the electrical wave hits this insulation it dies out and the
cells await the next impulse from the sinus node. The atria and
ventricle are electrically connected to one another by the
atrioventricular node (AV node). This conducts the electrical
wave slowly through from atria to ventricles giving the atria
time to contract before it then sends the impulse out through
the bundle branches (BB ? electrical ?motorways? that spread
the electrical wave very quickly through the ventricle) and
the ventricles causing them to contract. Once a heart cell has
been excited by an electrical wave it takes a few tenths of a
second to recover before it can be excited again so whatever
area it passes through is unexcitable for a short time. The
wave therefore washes through the heart from top to bottom
before dying out, until the next impulse from the
SN. In AF rather than
a single electrical wave emerging from the Sinus Node there
are lots of smaller waves which are continuously wandering
around the atrium. The path that these waves take and the
number of waves that there are is limited by the amount of
excitable tissue in front of each wave front. If one wave hits
an area of the heart that another wave has just excited it
cannot continue because the tissue has just been excited and
is unexcitable. It therefore either changes direction, splits
into 2 waves and passes around the unexcitable tissue or dies
away. To see a recording of atrial fibrillation in a human
click here. This is a recording made over a period of a 10th
of a second with a mapping system called non-contact mapping
and is of a human left atrium. The video shows 2 views of the
left atrium (front and back) with electrical waves as white
and coloured areas passing over the surface of the atrium
(coloured purple when not being activated). In this recording,
which is slowed down to help the viewer see a bit of what is
going on, one can see how complex atrial fibrillation
is. Most often atrial
fibrillation originates in the left atrium but will affect
both the left and right atrium because they are in electrical
continuity. Therefore in the film you have just seen the waves
that appear from nowhere have probably just broken through
from the right atrium to the left atrium. The AF waves are
therefore continuously moving around the atria which means
that the atrial cells are contracting in a chaotic fashion.
This means that the atria does not contract but appears to
shiver or fibrillate. This has 2 important effects, firstly
the atria do not squeeze blood out of the many cul-de-sacs
that exist within the atria which may allow blood to stagnate
or in high risk people, clot. If clots form in the left atrium
then they may be dislodged and fly off into the circulation.
One of the biggest destinations of blood from the heart is the
brain, so if clots are carried away by the circulation they
may reach the brain and cause a stroke. Stroke risk can be
reduced by giving high risk patients warfarin and low risk
patients aspirin. For a list of
patients at high risk of stroke and the level of
anticoagulation they should get click here. The other effect
that the lack of atrial contraction has is to reduce the
efficiency of the heart. The atria can be likened to a
turbo-charger on a car. If your car is sitting at the traffic
lights it does not use the turbo. The effect of the atrial
contraction is similarly minimal when someone is resting,
because all the blood flows into the ventricle on its own
without the atrium. However when the traffic lights go green
and the driver puts their foot on the pedal they will notice
immediately that the turbo is not working because the car will
be much slower than normal. The same is true for the heart,
particularly in active people. Many patients notice that they
are in AF because they cannot do as much as they could when
they were in normal rhythm. Obviously in people who normally
do very little physical activity like the very elderly and the
infirm, they will never use the atrial part of their heart
function and so may not notice this effect. Because AF is a
chronic condition, patients get used to this lack of function
and forget what it was like when they were in normal rhythm.
It is not uncommon for patients to be surprised at what they
can do when restored to normal rhythm and feel worse if they
return to AF because they are reminded what it is like to be
in normal rhythm. It is important
to remember that the atrium is insulated from the ventricle so
that ventricle is not directly affected by these waves.
However there is a connection between the atria and
ventricles, the AV node. When an AF wave passes across the AV
node, if it is excitable (and hasn?t already just been
activated by a wave), it will conduct to the ventricles and
make them contract. Because this process is chaotic and
random, because the AF waves follow a random path, activation
of the AV node and thus the ventricles is random and
irregular. Therefore one of the symptoms patient?s experiences
is an irregular heart beat. The atria are too small for you to
feel the effect of their contraction but the ventricle is
strong enough for you to feel so when you feel your heart is
irregular during AF it is the ventricles response to the atria
that you are feeling, not the atria themselves. The AF waves
are continuously passing around the atria rather than emerging
once a second from the Sinus Node so the AV node is excited
more often than normal so not only does the heart feel
irregular but also faster than normal. How common is Atrial
Fibrillation (AF) ? AF occurs in a
approximately 1 in 100 people. It gets more common as one gets
older and in the population over 75 years of age it occurs in
10% of the population. Many patients try
to find reasons why their AF has started and look for things
they do that have triggered it. There is often no trigger that
you have caused so do not blame yourself. Things that are
strongly associated with AF are excessive alcohol,
particularly binge drinking, other cardiovascular disease
particularly heart valve disease and high blood pressure and
thyroid gland disease. There is an almost infinite number of
things that may trigger AF in individual patients but common
things are exercise, reflux of acid into the oesophagus
(heart-burn) and stress/anxiety. In patients with no heart
disease or cause for their AF (common situation) it is called
?lone AF?. Common symptoms
are: 1. Palpitation ?
a feeling that ones heart is racing or going faster than
normal 2. Lethargy
because the ?turbo-charger? of the heart is not
working 3. Shortness of
breath 4. Dizzy spells
or fainting? because the heart can go too fast or too slow,
preventing it from pumping blood efficiently and thus dropping
the blood pressure 5. Chest
pain 6. Symptoms of
stroke ? transient or permanent weakness of an area limited to
one side of the body What are the
signs of AF? You may notice
that your heart is continuously irregular or unexpectedly
fast. The heart rate rises naturally when you exercise but
should not be faster than 90 beats per minute if you have been
resting for a while. Many patients may not realise they have
AF until someone takes their pulse, for example at a routine
medical examination. What are the
risks of AF? Traditionally AF
has been considered a benign heart rhythm, i.e. it is not
dangerous. Unfortunately this is a belief still held by some
doctors who have not kept up to date with research. AF has the
following dangers associated with it: 1. Stroke - AF is
the commonest cardiac cause of stroke for reasons explained
under What is Atrial Fibrillation? above. Certain
people are at high risk of stroke. This risk can be reduced by
warfarin in high risk patients and aspirin in low risk
patients. Many doctors under-prescribe warfarin because they
feel that the elderly who are most at risk of stroke, may be
at risk of falling and the bleeding because of the warfarin.
Many patients refuse to take warfarin because they are
concerned about the inconvenience of the regular blood tests
and do not understand the risk of stroke and the devastation
it can cause. There are newer drugs under trial at the moment
that avoid the need for regular blood tests but there are
currently problems with these because of potentially serious
side effects. It will therefore be some time until they are
fully tested and available. 2. Heart failure
? AF can cause heart failure by making the heart beat too
quickly. If you were asked to run on a treadmill at a fast
rate you would become tired pretty quickly. If you ask the
heart to beat at a fast rate then it will also get tired. Good
heart rate control both at rest and during exercise is
therefore important. There is evidence emerging that heart
failure can occur in some patients despite good rate control
and that restoration of normal rhythm by catheter ablation can
help the heart to recover. 3. Death ? no one
truly understands why patients with AF die but a number of
studies have shown that even when you correct for other
diseases patients with AF are more likely to die than patients
in normal rhythm. The largest study of this effect, the
Framingham study showed that AF doubled peoples mortality
rates. Because we do not know why this happens we cannot be
sure that any treatment we give will prevent it so although it
seems likely that restoration of normal rhythm will reduce the
chances of death there is currently no proof that this is the
case. Benjamin
EJ, Wolf PA, D'Agostino RB, Silbershatz H, Kannel WB, Levy D.
Impact of atrial fibrillation on the risk of death: the
Framingham Heart Study. Circulation. 1998 Sep 8;98(10):946-52
The most important thing is to confirm whether you do have
AF or not. This is done by recording the electrical activity
of the heart during your symptoms (or when your heart is fast
and irregular if you do not have symptoms). Recording the
electrical activity of the heart is called an
electrocardiogram (ECG). This can be done either in a doctors
surgery on a fixed machine, on a treadmill during an exercise
ECG or with a device that you can carry around at home using
either a Holter monitor or event recorder. It is also
important that someone competent looks at the results. Even
cardiologists who do not specialise in heart rhythm problems
may get it wrong. If AF has been confirmed then you should have some simple
tests to check that there is not an underlying cause for it.
You therefore should have had: 1. your blood pressure measured to exclude hypertension
(high blood pressure) 2. your thyroid function measured with a blood test 3. an echocardiogram to exclude structural heart disease
that is sometimes impossible to detect with an examination Once other causes for AF have been excluded or treated then
you must make a decision as to how you want your AF treated.
If you opt to accept AF and simply have you heart rate
controlled, recording the ECG during exercise or with a 24
hour Holter recording will give a much better idea of what
your heart rate control is with just one examination at
rest. When deciding
what treatment to have for your AF it is important to remember
that no treatment is without risk associated with it. This
includes tablets and operations. When doctors are advising on
treatment we are trying help you assess what is the best
option for you based on the risks and benefits of each
therapy. Doctors are trying to predict how things may turn out
for you based on statistics, research and their experience of
other patients but inevitably until doctors can see into the
future we will not always get it right. Obviously the more
patients with AF we see and the more research we do the better
our advice is likely to be. Essentially there
are 3 problems associated with AF that need
treating: 1. stroke
risk 2. fast heart
rate 3. abnormal
irregular rhythm 4. Catheter
Ablation For details go
here What is the Outcome of Atrial
Fibrillation? This material is used
with the kind permission of The London Atrial Fibrillation
Centre http://www.londonafcentre.co.uk/
Visit this site as there
is more information available
there.
What is Atrial
Fibrillation?
The
anatomy of the heart
The conduction system

Why does Atrial
Fibrillation Happen?
Atrial Fibrillation
Symptoms, Signs and Risks
Atrial
Fibrillation Investigations, What Tests Should I
Have?
Atrial Fibrillation
Treatment options
Contrary to
popular belief AF is not benign. The mortality rate rises by
up to 1.9 times in patients with AF, the reason for which we
do not know. There have been a number of studies examining
whether restoring sinus rhythm is better than just controlling
rate in AF and these have all shown that controlling rate is a
policy that is as good or better than controlling rhythm.
HOWEVER these studies all examined conventional (drugs and
cardioversion) methods of treatment and many of the patients
in the rhythm control group failed to stay in sinus rhythm.
Furthermore anticoagulation was stopped too soon and many
patients who went back into AF suffered stroke. It has been
shown that if the patient does stay in sinus rhythm they have
a lower mortality than those in AF and there is early evidence
that catheter ablation can reduce mortality and improve
patient symptoms. Because this is a relatively new technique
for treating AF more thorough evidence is yet to be collected
to demonstrate whether catheter ablation eliminates the
mortality risk of AF.


